UCSF Scientists Use Human Stem Cells to Generate Immune System in Mice
Raising hopes for cell-based therapies, UCSF researchers have created the first functioning human thymus tissue from embryonic stem cells in the laboratory.
University of California San Francisco
Give to UCSFRaising hopes for cell-based therapies, UCSF researchers have created the first functioning human thymus tissue from embryonic stem cells in the laboratory.

Shinya Yamanaka's Nobel Prize for stem cell research brought fresh attention to something UCSF long ago sensed and seized: the promise of regeneration medicine for repairing or replacing damaged cells, tissues, and even whole organs.

UCSF recently convened experts to discuss cell therapies, which have already saved children and adults from leukemia in clinical trials after other drugs failed them.

UCSF scientists have discovered that muscle repair requires the action of two types of cells better known for causing inflammation and forming fat.
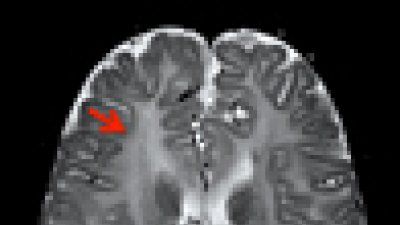
Specific DNA once dismissed as junk plays an important role in brain development and might be involved in several devastating neurological diseases, UCSF scientists have found.
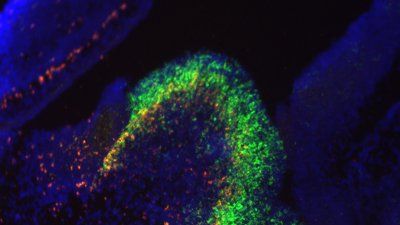
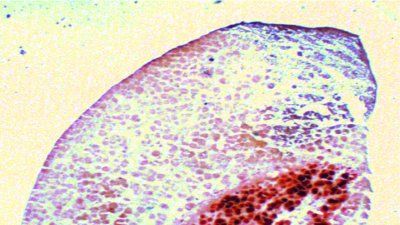
Treating patients with cells may one day become as common as it is now to treat the sick with drugs made from engineered proteins, antibodies or smaller chemicals, according to UC San Francisco researchers who have outlined their vision of cell-based therapeutics as a “third pillar of medicine."

Scientists at UC San Francisco will host a one day symposium, “Cell-Based Therapeutics: The Next Generation of Medicine,” with some of the nation’s leading clinical and laboratory researchers in stem cell therapy, immunotherapy and bacterial therapeutics.

Stem cells of the aging bone marrow recycle their own molecules to survive and keep replenishing the blood and immune systems as the body ages, UCSF researchers have discovered.

<p>The California Institute for Regenerative Medicine has awarded $12 million in stem cell research grants to fund four projects at UCSF, part of a total $36 million in new awards to young researchers announced by the state agency.</p>

<p>Shinya Yamanaka, MD, PhD, and John Gurdon, PhD, are in Stockholm this week to receive the 2012 Nobel Prize in Physiology or Medicine for their discoveries that led to the development of induced pluripotent stem cells.</p>

<p>Stem cell “banks” could serve as a valuable resource for emerging treatments in the field of regenerative medicine, though challenges remain to making them a reality, according to international experts who recently gathered at UCSF.</p>
<p>Weeks after winning the 2012 Nobel Prize in Medicine, Shinya Yamanaka, MD, PhD, and John Gurdon, PhD, were able to celebrate their monumental achievement together for stem cell discoveries made half a century – and half a world – apart.</p>

<p>When Shinya Yamanaka won the Nobel Prize in Medicine, colleagues at UCSF and the Gladstone Institutes and scientists from his lab gathered Monday afternoon to cheer the laureate and raise champagne toasts, while he shared in the celebration via live video streaming from halfway across the globe.</p>


<p>A new study that represents a significant first step in exploring the potential of stem cells to treat neurological disease is a “natural outgrowth” of a longstanding culture of interdisciplinary collaboration in UCSF neonatology — a culture that UCSF Benioff Children's Hospital physicians David Rowitch and Donna Ferriero work hard to sustain.</p>

For the first time, a clinical trial led by UCSF investigators and sponsored by Stem Cells Inc., has shown that transplanted neural stem cells appear to produce myelin in the brains of four young children with an early-onset, fatal disease.