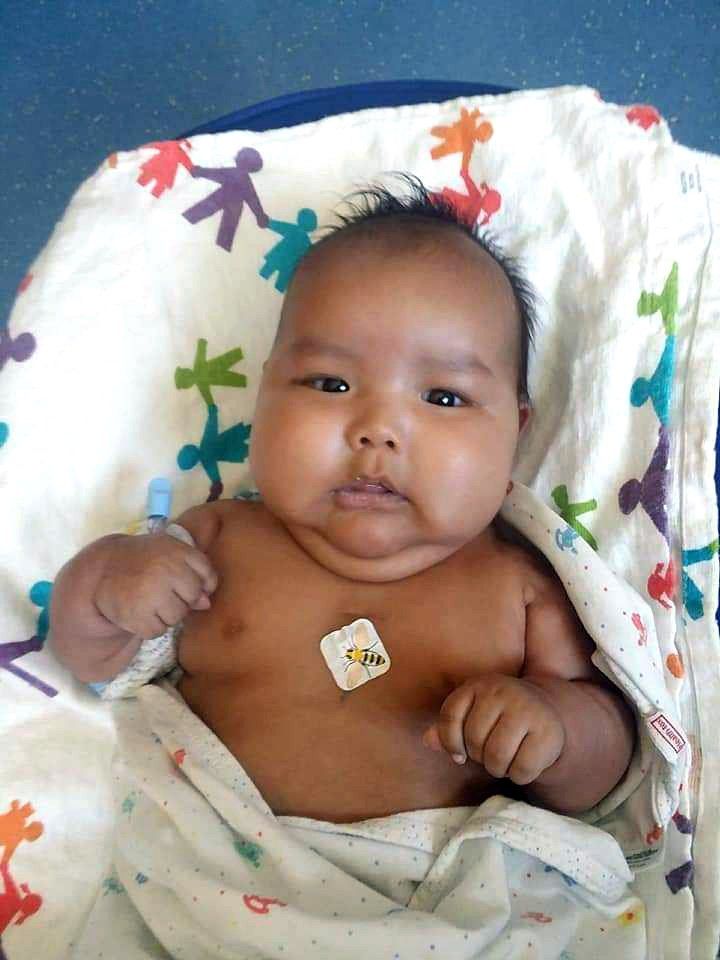
When Hataalii Tiisyatonii Begay was born on April 7, 2018, his family members rejoiced in the hospital in Tuba City, Ariz., and on the remote Navajo Nation reservation where they lived. With his shock of black hair and shining black eyes, Hataalii quickly won over everyone he met.
His parents called him ‘HT’ for short. “He was a beautiful baby, and we were all excited that he came into the world,” said Laverna Shorty, his paternal grandmother.
Within days, however, the family’s exuberance gave way to fear. Doctors at Tuba City Regional Hospital had found something abnormal in HT’s blood tests, and he needed to be airlifted to Phoenix Children’s Hospital for more tests.
“The pediatrician told us it was very serious and HT needed to be kept in isolation as a precaution,” said Shorty. “When you hear something like this about your child, your world kind of stops.”
It would be years before it felt like the world started up again.
Bubble Baby Disease
HT was found to have a rare mutation in the DCLRE1C or Artemis gene, meaning he had Artemis-SCID – the most serious of primary immunodeficiencies, otherwise known as Bubble Boy or Bubble Baby Disease (females can have it too).
Children with Artemis-SCID lack a functioning immune system and are highly susceptible to infections, which often accumulate and become severe, even deadly. They are frequently plagued with a poor quality of life due to repeated and persistent infections, chronic diarrhea, and failure to gain weight. Most die before 1 year of age.
The standard treatment for Artemis-SCID is a bone marrow transplant from a donor, ideally a matched sibling.
Back in Phoenix, doctors tested the blood of HT’s brother and parents to see if they were a match and awaited the results, which would take several weeks.
“When I went to Phoenix to visit HT, I had to scrub my hands up to my arms and wear a gown and mask,” Shorty said. “They told us the best hospital for SCID was UCSF, but HT needed to be a little older before it was safe to airlift him.”
HT was in the Phoenix hospital for about a month.
“He was really sick. He had norovirus; he couldn’t nurse and had to be on a bottle, but even then, he wouldn’t latch on,” Shorty said.
Lives Transformed: Laverna Shorty describes her grandson HT’s journey while Drs. Mort Cowan and Jennifer Puck discuss the research that led to this clinical milestone. Video produced by Gillian Grisman
First in the World
With the results of the bone marrow tests still pending, HT was airlifted to UCSF with his parents to meet pediatricians Mort Cowan, MD, and Jennifer Puck, MD, internationally known experts in researching and treating SCID.
“Artemis-SCID is one of the hardest genotypes of SCID to treat,” noted Cowan. “When you don’t have a matched sibling, it has only about a 50% survival rate even with modern transplant technology. Four out of five times, there isn’t a sibling match for marrow, and you have to find an alternative donor, which typically means more severe complications and more intense therapy.”
As luck would have it, Cowan and Puck had just embarked on a Phase I/II clinical trial for a new kind of Artemis-SCID treatment that involved transplanting a child’s own gene-corrected stem cells, rather than a donor’s.
Gene correction had been used with other genetic forms of SCID but attempting it with Artemis-SCID was riskier. Artemis-SCID patients usually respond more poorly to standard bone marrow transplants than other SCID patients, with complications ranging from marrow graft rejection to premature death. At UCSF, HT’s family learned that neither his brother nor his parents were a match. He was put on a waiting list for an unrelated donor match. Cowan and Puck offered the clinical trial as an alternative.

“We had a big Zoom call about it – HT’s parents, all his grandparents, his Arizona doctors, and Dr. Cowan and Dr. Puck.” Shorty said. “Then the family prayed and talked about it. HT was pretty sick, and we didn’t think we could wait for a match. So, we decided to go with the trial.”
The procedure happened on June 23, 2018, and went off without a hitch. HT was the first child in the world with Artemis-SCID to receive gene-correction therapy.
“They agreed to be pioneers for this treatment,” Cowan said. “They really led the way.”
The Clinical Trial
HT was the first of 10 Artemis-SCID babies to be safely transfused with their own gene-corrected stem cells as part of a Phase I/II clinical trial reported in the Dec. 22 issue of New England Journal of Medicine.
By 12 weeks, all the patients had begun growing their own T cells and B cells, which are critical for healthy immune systems. Four of the 10, including HT, achieved full B cell immunity by 24 months and no longer needed regular immunoglobulin infusions to stay healthy. They were also able to receive standard childhood vaccinations.
An additional three patients, who were followed for fewer than 24 months at the time of publication, have promising B cell development when compared to previous outcomes for donor-transplanted patients.
All 10 children are now living with their families, going to preschool or daycare, and living normal lives, said Mort Cowan, UCSF pediatrics professor and lead researcher. “Already, the course of their illness is so much better than with the typical treatment. I’ve treated more than 30 children with Artemis-SCID, and I’ve never seen results like this in any of the other kids.”
Prayer and Full-Time Care
Now came the recovery – in some ways, the hardest part. “We believed that the treatment would work, but we knew it wouldn’t happen right away,” Cowan said. “It takes about three months for a stem cell to grow into a T cell. That’s a long time to wait in isolation.”
During this period, Shorty decided to take over care for HT, freeing up his parents to work and keep the family on their health insurance. She flew to San Francisco and got a crash course in medical terminology – all in English, her second language.
“At first, I was cautious to touch him because of his PICC line,” said Shorty, referring to an IV that is inserted into a vein in the arm, then threaded into a large vein in the chest. “After a while, I learned how to draw his labs, flush his PICC line, and administer meds. I became Grandma Nurse.”

Sleeping on a couch that converted to a bed, she largely lived in isolation with HT. She barely left his side and never stopped praying to have faith in Western medicine. One night, after months spent listening to music, watching cartoons, and rocking HT in her arms as she danced, Shorty was overcome with anxiety and felt claustrophobic.
“I paced the hallway and a security guard saw me, took me to sit outside and brought me a cup of coffee. That’s the moment I fully realized the disease HT had, and that it would take a lot of time to help him; it wouldn’t happen overnight,” Shorty said. “There would be days where all we could do was see if his body accepted the treatment.”
A month after his transplant, HT developed his first three T cells, and the doctors and family celebrated, naming two of the cells after HT’s great grandparents, Jack and Willy. The third, in a moment of giddiness, was simply named Fred.
Finally, on Nov. 26, 2018, HT was healthy enough to be discharged from the hospital to outpatient care with weekly clinic visits for immunoglobulin infusions. Shorty and HT moved to Family House, a nonprofit that provides temporary housing near Benioff Children’s Hospital San Francisco for families of seriously ill children while they receive treatment.
Life Outside the Bubble
There were many ups and downs over the next three years – bouts of neutropenia, eczema, anemia and mouth sores, all common ailments for Artemis-SCID patients. During that time, HT and Shorty connected with other families, sharing coffee and play dates.
“I met families who had babies with all kinds of different diseases, like cancer. I just started reaching out to them. I even met a family from Guam whose baby had SCID,” Shorty said.
Among milestones big and small, one sticks out in her mind: Sept. 26, 2019, when Cowan and Puck gave HT permission to play outside in the dirt for the first time. It was something commonplace for other kids, but for HT it meant his immune system had rebuilt itself enough so that he could venture outside his bubble.
For Shorty, it was an important step toward the outdoor life at the reservation that she hoped HT would one day return to.
“Inside, HT liked Legos and puzzles, blowing bubbles, and books,” said Shorty. “But when we got the news he could go outdoors, we let him explore and to this day, he loves being outside the most of all.”
Though they were adapting, Shorty and HT still missed their people and their home in Arizona.
“I thought about my family every day, praying for HT’s recovery and hoping soon, HT would be okay and we could go back for good.”
Journey Home
After a false start in December 2021, when HT went home but a bout of anemia quickly sent him back to UCSF – HT finally moved back to Arizona in April 2022. Now, he comes to UCSF for check-ups twice a year.
“HT is a very happy-go-lucky guy,” said Cowan. “He’ll just march right into the exam room and give you a high five. He’s inquisitive, sociable and very fun to be around.”
Nowadays, HT is off his medication and living the life of a normal and happy young child. On the Arizona ranch, there are horses to pet, cattle and sheep to tend, and streams to cool his hands in. In the mornings, HT gathers chicken eggs with his older brother as his father looks on.
When weather or darkness forces him inside, HT plays with toy dinosaurs and Tonka cars. But his favorites are his toy airplanes.
“He wants to be a pilot when he grows up; he wants to fly from Arizona to San Francisco,” said Shorty. “And he says he is going to take his grandma with him everywhere he goes.”
