Human Proteins Behind COVID-19 Infection Revealed by Innovative CRISPR Technology
Existing Drug May Block the Virus, But Side Effects are Unknown
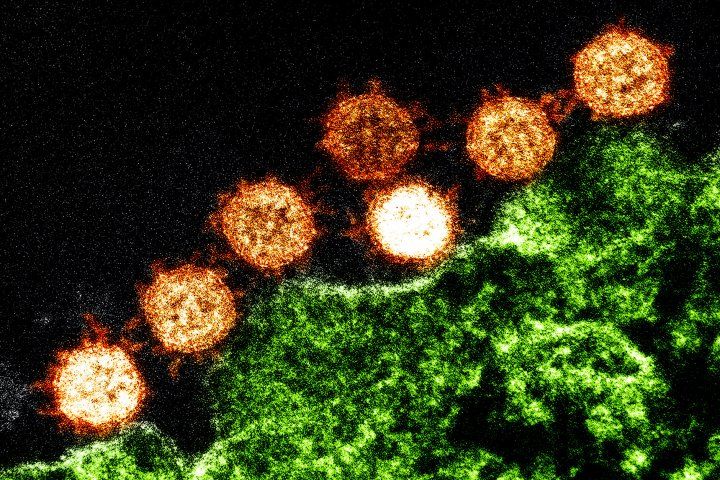
In the quest for new treatments for COVID-19, a team led by researchers at UC San Francisco has identified a new potential drug target that may block infection by SARS-CoV-2. The protein, called BRD2, regulates the ACE2 receptor, which the novel coronavirus relies on to gain entry to its host’s cells.
In their new study, published Jan. 13 in Nature Cell Biology, the researchers found that blocking production of BRD2 prevents the virus from infecting a variety of human cell types.
“We’ve known that BRD2 regulates expression of other genes, including those that help promote tumor growth in some cancers,” said Martin Kampmann, PhD, an associate professor of Biochemistry and Biophysics and senior author on the study. “Having discovered how the protein regulates ACE2 means that pathway could potentially be manipulated to make it harder for SARS-CoV-2 to infect cells.”
Unlike many of the proteins being studied as potential targets against COVID-19, BRD2 isn’t produced by the virus, but by the cells of its human host. The protein and others related to it are currently being investigated in clinical trials as targets for cancer drugs.
Focusing on ACE2’s Gatekeeper
The researchers discovered that BRD2 regulates ACE2 while searching for human host proteins that affect the ability of SARS-CoV-2 to attach to various cell types grown in lab cultures, including cells from lungs, heart, and nasal cavity – tissues especially susceptible to infection and long-lasting damage due to COVID-19.
Repressing genes and their products with CRISPR can mimic their inhibition by drugs and uncover which drug targets may be therapeutically beneficial.
The scientists screened 2,325 cellular proteins that they thought might affect COVID-19 infection by influencing the virus’s interaction with human cells. They determined that existing drugs targeting BRD2 can thwart COVID-19 infection in susceptible cell types, as well as in hamsters.
“We were amazed to see that knocking down BRD2 has almost the same effect on inhibiting ACE2 production and COVID-19 infectivity as directly knocking down ACE2 itself,” Kampmann said.
The research team also included Avi Samelson, PhD, a postdoctoral fellow in Kampmann’s lab, and Ruilin Tian, PhD, a former graduate student in the lab who is now an assistant professor at the Southern University of Science and Technology in Shenzhen, China. They, along with other members of the Kampmann lab, which is usually focused on neuroscience, proposed the study out of a desire to contribute to a better understanding of COVID-19. Working with members of the Coronavirus Research Group of UCSF’s Quantitative Biosciences Institute (QBI) and collaborators recruited from around the world, the team identified several other cellular proteins that are potent enhancers and inhibitors of ACE2 production.
However, the researchers caution that this new study is only a first step, and many more studies will be required to prove the safety and efficacy of any drug directed at BRD2 or other newly identified targets.
For example, the team found that inhibiting BRD2 also inhibited the production of interferon, a key protein in the body’s inflammation response.
“It’s important to learn more about these potential side effects,” said Samelson. “We don’t know whether this impact on the immune system would be harmful or beneficial for an infected patient, and under what circumstances.”
CRISPR Aids Drug Target Search
Kampmann is known for inventing innovative new lab techniques based on the powerful gene-editing technology, CRISPR, which was engineered from unique biochemical machinery used by bacteria to fight viruses that infect them.
Scientists first used CRISPR less than a decade ago, to direct the cutting of DNA at specific sites along the genome and now employ the technique to edit DNA in a wide range of organisms.
Kampmann and his colleagues have modified the original bacterial enzyme used in CRISPR so that rather than cutting DNA, it ferries regulatory molecules to specific sites within the genome. Once there, these regulatory molecules can activate or repress genes, overriding normal gene expression.
This ability to fine-tune the gene expression up or down is a useful approach for identifying drug targets, Kampmann said. “Repressing genes and their products with CRISPR can mimic their inhibition by drugs and uncover which drug targets may be therapeutically beneficial.”
Another benefit is that these CRISPR screenings are unbiased, meaning that the researchers aren’t looking for a particular outcome, but methodically testing each protein to see which ones have the desired effect, said Tian, who aims to continue studying COVID-19 in China.
“Using this powerful approach helps us to find many potential targets that we might otherwise not see,” he said. “In doing so, this screening helps facilitate new strategies to fend off infection by SARS-CoV-2 and its variants.”
This research was supported by NIH grant F32AG063487 and fellowships.
Authors: For additional authors, please see the study.
The University of California, San Francisco (UCSF) is exclusively focused on the health sciences and is dedicated to promoting health worldwide through advanced biomedical research, graduate-level education in the life sciences and health professions, and excellence in patient care. UCSF Health, which serves as UCSF’s primary academic medical center, includes top-ranked specialty hospitals and other clinical programs, and has affiliations throughout the Bay Area.