Vaccine Hesitancy in Young Adults May Hamper Herd Immunity
Questions About Safety, Side Effects Preclude Youth from Getting COVID Shot, UCSF Study Shows
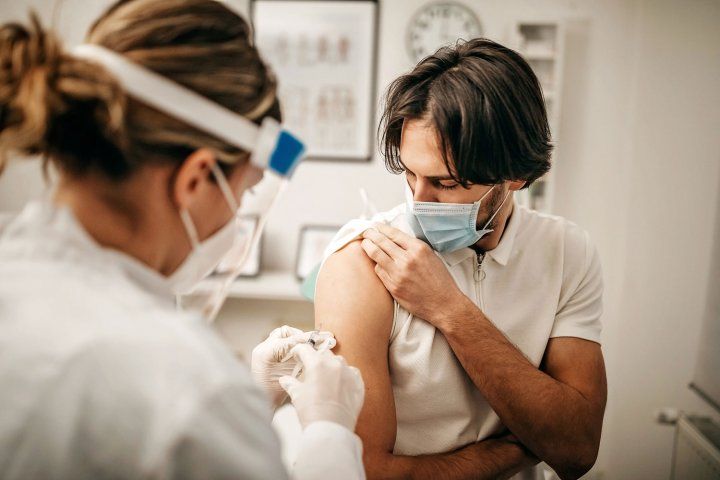
Vaccine skepticism among young adults may stall efforts to achieve herd immunity – a threshold in which approximately 80 percent of a population is vaccinated against the coronavirus.
A study by UC San Francisco researchers found that about one in four unvaccinated people aged 18 to 25 said that they “probably will not” or “definitely will not” get the COVID-19 vaccination, despite the fact that this demographic has been found to be more likely than other age groups to transmit coronavirus, jeopardizing the health of older unvaccinated adults and facilitating the rise of virulent vaccine variants.
The researchers analyzed March 2021 data from the Household Pulse Survey, an online nationally representative sample of the population conducted by the U.S. Census Bureau in collaboration with the National Center for Health Statistics and other agencies.
Among the 5,082 respondents, 83 percent reported that they had not been vaccinated, 10 percent said they definitely will not get the vaccine, and 14 percent said they probably will not. The study appears July 14, 2021, in the Journal of Adolescent Health.
While data from the Centers for Disease Control and Prevention (CDC) show that very few 18 to 29-year-olds die of COVID-19 relative to older adults, this age group accounts for more than 20 percent of all COVID-19 cases to date. Furthermore, previous research by lead author Sally Adams, PhD, RN, of the UCSF National Adolescent and Young Adult Health Information Center, found that as many as one in three young adults is at risk of severe COVID.
‘Long COVID’ May Impact Young Adults Even With Mild Symptoms
“Young adults who have had COVID, regardless of symptoms, may be vulnerable to long-term complications and debilitating symptoms that may include respiratory difficulties, loss of smell and brain fog, often referred to as ‘long COVID.’ Estimates range from 10 to 50 percent for long COVID symptoms, which is a serious concern for young adults given their high infection rates and low vaccination rates,” Adams said.
“Prompt vaccinations could help limit the further development of virulent variants and infection rates among the vulnerable and unvaccinated,” she added.
Among the unvaccinated respondents who said they would definitely not or probably not get the vaccine, more than half said they were concerned about possible side effects. Half said they planned to wait and see if the vaccine was safe and may get it later. Also, within this group, a third said that they do not trust the vaccine, compared to fewer than one in 10 of those who said that they probably would get vaccinated.
The recent spate of heart inflammation cases in teens and young adults following the Pfizer and Moderna vaccines may have amplified many people’s fears, said senior author Charles Irwin Jr., MD, director of the Division of Adolescent and Young Adult Medicine at UCSF Benioff Children’s Hospitals.
“It’s important to note that the rate of heart inflammation in young people who have been vaccinated is only slightly higher than in young people who have not been vaccinated. In most cases, symptoms are mild and resolve with minimal treatment,” said Irwin. “As a result, the majority of providers support the CDC and other advisory bodies that continue to recommend the vaccine for everyone age 12 or older.”
The researchers recommend that young adults’ concerns about vaccine safety and side effects are addressed via public education campaigns. “Education and public health messaging encouraging young adult vaccination is needed, ideally harnessing social media and key influencers,” Irwin said, “including clinicians who have a key role in reducing vaccine hesitancy in youth and adult patients.”
UCSF Benioff Children’s Hospitals are two leading Bay Area children’s hospitals with longstanding commitments to public service. UCSF Benioff Children’s Hospital San Francisco and UCSF Benioff Children’s Hospital Oakland both have leading pediatric residency programs, unique pediatric subspecialty fellowship programs, a research base for the next generation of discoveries, and expertise in pediatric clinical care, public policy and patient advocacy.