COVID-19 Vaccine Fact Vs. Fiction: An Expert Weighs in on Common Fears

Mel Hirschkorn Sr. (left) receives his first dose of the Moderna COVID-19 vaccine from UCSF nurse Patrick Sorensen, RN, at a vaccination drive-through at City College San Francisco. Photo by Susan Merrell
As global COVID-19 cases top 100 million, health experts are emphasizing the urgency of vaccinating as many people as possible to stop the spread. More circulating virus means the more likelihood of mutations, and some new variants already appear to be more contagious – making vaccination even more of a race against time.
But with vaccines developed at unprecedented speed and a virus still revealing its ways, people understandably have many questions about the new vaccines.
We posed the most common COVID-19 vaccine quandaries to Bryn Boslett, MD, an infectious disease expert who is leading the vaccination effort at UC San Francisco. She explains why mRNA vaccines won’t affect your DNA, which allergies pose a risk, what 95 percent efficacy really means, and more.
Do the mRNA vaccines change your DNA?
Both the Pfizer and Moderna vaccines are mRNA vaccines, which means they contain messenger ribonucleic acid. “It’s basically a piece of material that contains instructions,” said Boslett. “Once it’s injected, it’s taken up by your cells, but it never enters the cell nucleus where all of your DNA exists within your cells.” The mRNA contains instructions for your cells to make spike proteins that match the ones found on the surface of the SARS-CoV-2 virus, which causes COVID-19. When your cells present these spike proteins on their surface, your body recognizes them as foreign and develops an immune response, including antibodies specific to the spike protein.
“The mRNA is a just temporary message,” said Boslett. “After the spike protein gets made, your body destroys the mRNA so it doesn’t stick around in the body. It doesn’t mix with any genetic code. It doesn’t go into your DNA. I’m not at all worried about there being any kind of damage to a person’s DNA from these vaccines.”
VERDICT: No.
Is immunity from the vaccine stronger than natural immunity from infection?
“The first time your body sees the spike protein, it activates some immune system cells to begin to recognize and develop antibodies against that protein,” said Boslett. The response may be similar whether that first encounter is from infection with the virus or from the first dose of the vaccine.
Studies of the mRNA vaccines suggest that one dose may offer between 50 to 80 percent protection against symptomatic COVID-19, though more data is needed, said Boslett. “We know you get some amount of protection after one dose of the vaccine or after infection with the virus, but we don’t know in either case how long that protection lasts,” she said. Some cases of reinfection have been reported after three to six months, so the protection from one dose of the vaccine also may wane in that timeframe.
“However, when you get the second dose of the vaccine, you’re further training your immune system,” said Boslett. “You’re strengthening that response from the antibody-producing B cells and you’re also activating T memory cells that stick around for much longer.” Getting both doses of the vaccine means your body is shown this spike protein multiple times in a short duration. “So that immune response might be bigger, better and longer lasting than just getting the infection one time,” she said.
Because the booster effect is so important, Boslett adds that this is why people who have had COVID-19 are still recommended to get the vaccine.
VERDICT: Probably.
Did the vaccine clinical trials skip steps to be completed faster?
Vaccine trials often take years because not only do they need to recruit a lot of participants to be able to evaluate safety and efficacy, they then need to wait for natural infections to take place. The COVID-19 vaccine trials have moved along faster thanks to extra financial support from the government and other funding sources, and the high prevalence of the virus in the community, said Boslett. “They didn’t skip any steps.”
More than 40,000 people were enrolled in the Pfizer vaccine trials, and more than 30,000 in the Moderna vaccine trials. “That’s a lot of people, but if the virus were rare, that still wouldn’t be enough people,” said Boslett. “But because the virus is running so rampant throughout the U.S. and other places in the world, this was actually a good number of people to show a difference between the vaccinated and unvaccinated groups.”
The mRNA technology, which has undergone years of study for other potential vaccines, was another time-saver. Compared to vaccines that use live viruses, mRNA vaccines are relatively easy to manufacture. “Virus is actually hard to grow,” said Boslett. “The fact that this wasn’t a live vaccine allowed the manufacturing to be a little bit simpler.”
VERDICT: No.
Was vaccine efficacy only measured in symptomatic COVID-19?
The reported efficacy rates of 94 or 95 percent are for symptomatic disease only. Because the clinical trials for Pfizer and Moderna did not require regular testing for COVID-19, they were not a good indication of how well the vaccine protects against asymptomatic disease (which account for some 40 percent of cases).
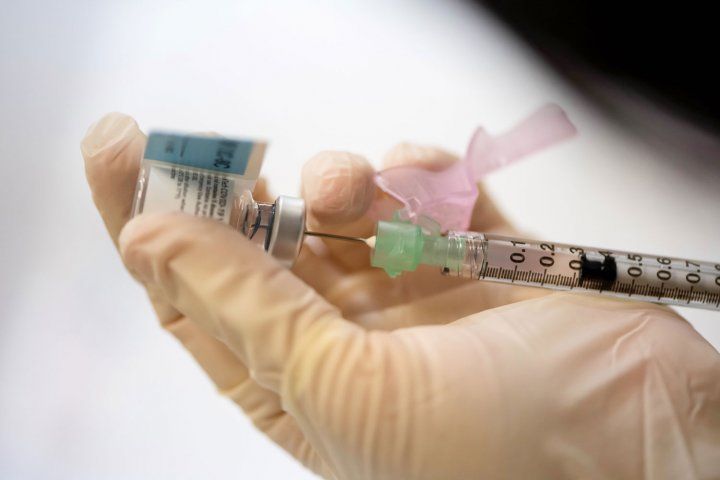
A dose of the Pfizer-BioNTech COVID-19 vaccine is prepared before it’s administered minutes later at the vaccine clinic at the Parnassus Heights campus. Photo by Susan Merrell
Limited data suggest the vaccines can prevent some asymptomatic infections. In the Moderna study, participants were tested just prior to receiving each dose. “There was a reduction in asymptomatic infection in the vaccine versus the placebo group, which gives us hope. Otherwise, researchers only found out that a participant got an infection if the person developed symptoms and then tested positive,” said Boslett. “We know the vaccine really reduces incidents of symptomatic disease, but we don’t know how it impacts the incidents of asymptomatic disease.”
Researchers should know the answer in a couple of months. “I think that logically speaking it should prevent or at least reduce asymptomatic disease,” said Boslett. “Most other vaccines do prevent both symptomatic and asymptomatic carriage and transmission, but until we prove it, we don’t want to assume anything.”
VERDICT: Yes.
Can the vaccine give you COVID-19?
Some vaccines, such as the measles or oral polio vaccines, contain a weakened form of the live virus, and in very rare cases these can cause disease. “But this isn’t one of those,” said Boslett. “The mRNA vaccines just contain a message that encodes the spike protein. It is not a live virus, so there’s no chance that the vaccine can give you COVID.”
Some people may feel symptoms such as fever or muscle aches after the vaccines, but those are due to your body’s immune response, not an infection. “That is actually not a bad thing because that means that your body is producing an inflammatory response to the vaccine, which is what we want.”
VERDICT: No.
If I have allergies, can I still take the vaccine?
You can safely take the vaccine with most allergies. “People who have allergies to food, pets, insect bites, latex, oral medications, environmental allergens, or even a family history of anaphylaxis do not have to avoid the vaccines,” said Boslett. According to the Centers for Disease Control and Prevention (CDC), people with these allergies have a low risk of having anaphylaxis (a severe, potentially life-threatening allergic reaction) in response to the COVID-19 vaccines and should still be vaccinated.
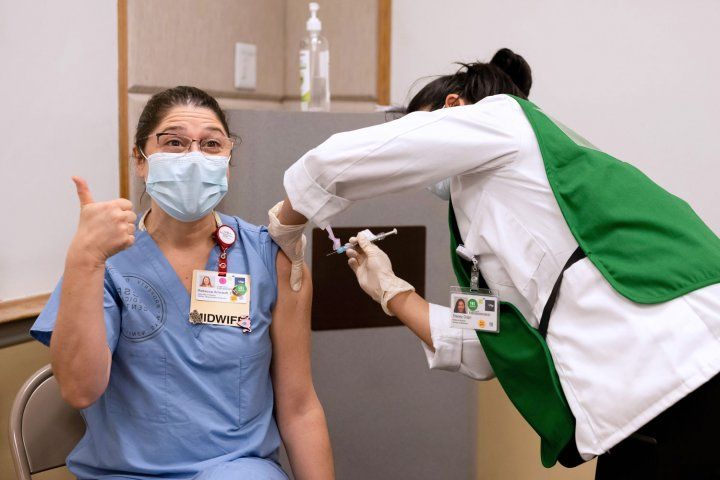
Rebecca Amirault (left), CNM, a UCSF professor and certified nurse midwife, celebrates receiving a COVID-19 vaccination from medical student Stacey Dojiri at the UCSF Parnassus Heights campus. Photo by Susan Merrell
If you’ve had a history of anaphylaxis to a non-COVID vaccine, then you may be at a slightly higher risk. “For those folks, it’s not necessary that you avoid the vaccine, but you might think twice about getting the vaccine right now. If you do get it, you want to wait at least 30 minutes for observation to see if you develop any type of response,” said Boslett.
If you’ve had a history of anaphylaxis to any components of the COVID vaccines, then you should not get the vaccine. If you experience a severe allergic reaction to the first dose of the vaccine, it’s recommended that you do not get the second dose.
“Less than a hundred out of the millions of people who have gotten the COVID-19 vaccines so far have had severe allergic reactions, so a severe allergic reaction is a rare event overall,” said Boslett.
VERDICT: Probably.
If I’m pregnant or breastfeeding, can I still take the vaccine?
“I would say it’s a very personal decision and should be something that every woman discusses with her medical team,” said Boslett. The American College of Obstetrics and Gynecology, the Society of Maternal Fetal Medicine, and the CDC have said that pregnant and breastfeeding women should be offered the vaccine when eligible.
“There’s no clear plausible reason to think that the vaccine would harm a fetus or a baby who’s breastfeeding in any way,” said Boslett. “This is not a live virus vaccine, and the mRNA is likely going to stay right in the arm where it’s injected and get taken up by the cells there. The mRNA is quickly degraded by the body after it does its job. We do not believe that the mRNA or spike protein will travel to the developing fetus or cause harm.”
A reasonable concern might be fever and other immune system reactions to the vaccine. “We know that in some cases, if a woman develops a high fever very early on in pregnancy, there have been some concerns historically over the contribution of fever to neural tube defects, but the evidence isn’t clear,” said Boslett. She recommends that if a woman develops fever after the vaccine, she should take Tylenol. “It’s not a reason to not get the vaccine, because if you think about it, if you get COVID, you may develop a fever and all kinds of other terrible immune responses. The vaccine is really protecting women against much more severe outcomes from COVID.”
It’s possible that women who are recently vaccinated may be able to pass some protective antibodies to the fetus through the placenta or to their baby through breastmilk, said Boslett. There is even ongoing research into extracting IgA antibodies from breastmilk to use for COVID-19 prevention in adults.
VERDICT: Yes.
Can you still transmit the coronavirus after vaccination?
This is another question that researchers are still investigating, said Boslett. “It’s possible that you could get the vaccine, have an immune response, but maybe not enough of an immune response to prevent asymptomatic infection, and still transmit the virus.”

Dipti Sil (right) receives her first dose of the Moderna COVID-19 vaccine from UCSF nurse Patrick Sorensen, RN, at a vaccination drive-through for San Francisco residents age 75 and older. Photo by Susan Merrell
Until proven otherwise, people should consider asymptomatic infections and transmission to be a possibility. “There’s a concern that people could get the vaccine and feel like they are safe, but they could be actually infected with the virus and carry it in their nasal passages and in their airways. And because they’re feeling safe, they might be less cautious and actually spread the disease,” said Boslett. With this in mind, health officials are urging everyone, even people who have received the vaccination, to continue to wear masks, stay six feet apart from people not in their own household and to wash their hands frequently.
The vaccines’ ability to prevent symptomatic disease is excellent, and will go a long way in preventing serious illness, hospitalizations and deaths. “But it’s not perfect,” said Boslett. “There were still a few people who, after two doses of vaccine, got infections. Whether that’s because their bodies just didn’t mount an appropriate immune response or something else, we don’t know.”
VERDICT: Maybe.
Will we need new vaccines if the virus continues to mutate?
“The amount of changes that we’re seeing in the coronavirus is not an overwhelming number of changes, but we do have these other variants coming out in the U.K. and in South Africa,” said Boslett. “At some point, could the number of mutations on the spike protein end up overwhelming what the vaccine can cover? I think that is possible.”
Whether we’ll need a new vaccine every year depends on how quickly we can get the pandemic under control. The likelihood of mutations depends on how much virus is circulating, said Boslett. “When there’s lots and lots of virus out there, that enables it to be inside of humans and make all kinds of little errors in its reproduction, and some of those mutations may end up helping the virus to spread.”
It’s also uncertain how long immunity from the COVID-19 vaccine will last. We need a flu vaccine every year not only because the flu virus mutates quickly but also because the antibody response wanes over time, according to Boslett.
The good news is that mRNA vaccines are relatively easy to adjust to target a new variant. (Moderna is already developing a new form of its vaccine aimed at the variant in South Africa, which could be given as a booster shot.) “I think that can be done in just two or three months,” said Boslett. “But how often we’re going to have to do that, I think remains to be seen.”
VERDICT: Maybe.