Brain Cells Most Vulnerable to Alzheimer’s Disease Identified by Scientists
Findings Could Lead to Targeted Treatments to Boost Brain’s Resilience
A major mystery in Alzheimer’s disease research is why some brain cells succumb to the creeping pathology of the disease years before symptoms first appear, while others seem impervious to the degeneration surrounding them until the disease’s final stages.
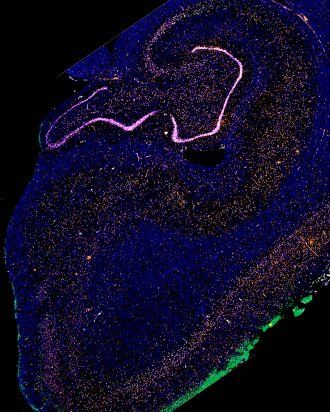
An image of human brain samples used to study why some brain cells are more vulnerable to Alzheimer’s disease than others. Image by Rana Eser, UCSF Grinberg lab
Now, in a study published Jan. 10, 2021, in Nature Neuroscience, a team of molecular biologists and neuropathologists from the UCSF Weill Institute for Neurosciences have joined forces to identify for the first time the neurons that are among the first victims of the disease – accumulating toxic “tangles” and dying off earlier than neighboring cells.
“We know which neurons are first to die in other neurodegenerative diseases like Parkinson’s disease and ALS, but not Alzheimer’s,” said co-senior author Martin Kampmann, PhD, an associate professor in the UCSF Institute for Neurodegenerative Diseases and Chan Zuckerberg Biohub Investigator. “If we understood why these neurons are so vulnerable, maybe we could identify interventions that could make them, and the brain as a whole, more resilient to the disease.”
Alzheimer’s researchers have long studied why certain cells are more prone to producing the toxic tangles of the protein known as tau, whose spread through the brain drives widespread cell death and the resulting progressive memory loss, dementia, and other symptoms. But researchers have not looked closely at whether all cells are equally vulnerable to the toxic effects of these protein accumulations.
“The belief in the field has been that once these trash proteins are there, it’s always ‘game over’ for the cell, but our lab has been finding that that is not the case,” said Lea Grinberg, MD, the study’s other senior author, an associate professor and John Douglas French Alzheimer's Foundation Endowed Professor in the UCSF Memory and Aging Center. “Some cells end up with high levels of tau tangles well into the progression of the disease, but for some reason don't die. It has become a pressing question for us to understand the specific factors that make some cells selectively vulnerable to Alzheimer’s pathology, while other cells appear able to resist it for years, if not decades.”
To identify selectively vulnerable neurons, the researchers studied brain tissue from people who had died at different stages of Alzheimer’s disease, obtained from the UCSF Neurodegenerative Disease Brain Bank and the Brazilian BioBank for Aging Studies, a unique resource co-founded by Grinberg. The São Paulo-based biobank collects tissue samples from a broad population of deceased individuals, including many without a neurological diagnosis whose brains nevertheless show signs of very early-stage neurodegenerative disease, which is otherwise very difficult to study in humans.
First, led by Kampmann lab MD/PhD student Kun Leng and PhD student Emmi Li, the study’s co-first authors, the team studied tissue from 10 donor brains using a technique called single-nucleus RNA sequencing, which let them group neurons based on patterns of gene activity. In a brain region called the entorhinal cortex, one of the first areas attacked by Alzheimer’s, the researchers identified a particular subset of neurons that began to disappear very early on in the disease. Later on in the course of the disease, the researchers found, a similar group of neurons were also first to die off when degeneration reached the brain’s superior frontal gyrus.
In both regions, these vulnerable cells were distinguished by their expression of a protein called RORB. This allowed researchers in Grinberg’s neuropathology lab, led by former lab manager Rana Eser, to examine RORB-expressing neurons in more detail in brain tissue from a larger cohort of 26 donors. They used histological staining techniques to examine the fate of cells from both healthy individuals and those with early and late stage Alzheimer’s. This work validated that RORB-expressing neurons do in fact die off early on in the disease and also accumulate tau tangles earlier than neighboring, non-RORB-expressing neurons.
“These findings support the view that tau buildup is a critical driver of neurodegeneration, but we also know from other data from the Grinberg lab that not every cell that builds up these aggregates is equally susceptible,” said Leng, who plans continue to study factors underlying RORB neurons’ selective vulnerability using CRISPR-based technology the Kampmann lab has developed.
It’s not clear whether RORB itself causes the cells’ selective vulnerability, the researchers said, but the protein provides a valuable new molecular “handle” for future studies to understand what makes these cells succumb to Alzheimer’s pathology, and how their vulnerability could potentially be reversed.
“Our discovery of a molecular identifier for these selectively vulnerable cells gives us the opportunity to study in detail exactly why they succumb to tau pathology, and what could be done to make them more resilient,” Leng said. “This would be a totally new and much more targeted approach to developing therapies to slow or prevent the spread of Alzheimer’s disease.”
Authors: Grinberg and Kampmann are both faculty members of the Department of Neurology in the UCSF Weill Institute for Neurosciences. Additional authors on the study were Antonia Piergies, Rene Sit, Michelle Tan, Norma Neff, Song Hua Li, Alexander Ehrenberg, William W. Seeley, and Salvatore Spina of UCSF; Roberta Diehl Rodriguez, Claudia Kimie Suemoto, Renata Elaine Paraizo Leite, and Carlos A. Pasqualucci of Universidade de São Paulo in Brazil; and Helmut Heinsen, of the Universidade de São Paulo and University of Würzburg in Germany.
Funding: The research was supported by the U.S. National Institutes of Health (NIH) (F30 AG066418, K08 AG052648, R56 AG057528, K24 AG053435, U54 NS100717); an NDSEG fellowship; Alzheimer’s Association fellowship (AARF 18-566005); Fundação de Amparo à Pesquisa do Estado de São Paulo and Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (FAPESP/CAPES 2016/24326-0); and a Chan Zuckerberg Biohub Investigator Award. The UCSF Neurodegenerative Disease Brain Bank is supported by the NIH (AG023501, AG019724) the Tau Consortium, and the Bluefield Project to Cure FTD.
Disclosures: The authors declare no competing interests.
The University of California, San Francisco (UCSF) is exclusively focused on the health sciences and is dedicated to promoting health worldwide through advanced biomedical research, graduate-level education in the life sciences and health professions, and excellence in patient care. UCSF Health, which serves as UCSF’s primary academic medical center, includes top-ranked specialty hospitals and other clinical programs, and has affiliations throughout the Bay Area.