UCSF, UCLA Gain FDA Approval for Prostate Cancer Imaging Technique
Method Is ‘Game Changer’ That Should Become Standard of Care, Say Researchers From Both Universities Who Validated Its Effectiveness

Thomas Hope (left), MD, and Peter Carroll, MD, chair of the Urology Department, stand at the PACS workstation where the images from the PSMA PETs are viewed and interpreted. The new imaging technique received FDA approval. Photo by Maurice Ramirez
The University of California’s two nationally ranked medical centers, UC San Francisco and UCLA, and their nuclear medicine teams have obtained approval from the U.S. Food and Drug Administration to offer a new imaging technique for prostate cancer that locates cancer lesions in the pelvic area and other parts of the body to which the tumors have migrated.
Known as prostate-specific membrane antigen PET imaging, or PSMA PET, the technique uses positron emission tomography in conjunction with a PET-sensitive drug that is highly effective in detecting prostate cancer throughout the body so that it can be better and more selectively treated. The PSMA PET scan also identifies cancer that is often missed by current standard-of-care imaging techniques.
“UCLA and UCSF researchers studied PSMA PET to provide a more effective imaging test for men who have prostate cancer,” said Jeremie Calais, MD, MSc, an assistant professor at the David Geffen School of Medicine at UCLA. “Because the PSMA PET scan has proven to be more effective in locating these tumors, it should become the new standard of care for men who have prostate cancer, for initial staging or localization of recurrence.”
A clinical trial conducted by the UCSF and UCLA research teams on the effectiveness of PSMA PET proved pivotal in garnering FDA approval for the technique at both universities. The PSMA drug used in the technique was developed outside the U.S. by the University of Heidelberg.
“It is rare for academic institutions to obtain FDA approval of a drug, and this unique collaboration has led to what is one of the first co-approvals of a drug at two institutions,” said Thomas Hope, MD, an associate professor at UCSF. “We hope that this first step will lead to a more widespread availability of this imaging test to men with prostate cancer throughout the country.”
How It Works
For men who are initially diagnosed with prostate cancer or who were previously treated but who have experienced a recurrence, a critical first step is to understand the extent of the cancer. Physicians use medical imaging to locate cancer cells so they can be treated.
PSMA PET works using a radioactive tracer drug called 68Ga-PSMA-11, which is injected into the body and attaches to proteins known as prostate-specific membrane antigens. Because prostate cancer tumors overexpress these proteins on their surface, the tracer enables physicians to pinpoint their location.
The current standard of care in prostate imaging is a technique called fluciclovine PET, which involves injecting patients with fluciclovine, a synthetic radioactive amino acid. Since prostate cancers consume more amino acids than normal prostate cells, the tumors accumulate large amounts of the synthetic tracer, making them easier to detect during scans.
In their research comparing PSMA PET and fluciclovine PET, the UCLA and UCSF research teams found that imaging with PSMA PET was able to detect significantly more prostate lesions than fluciclovine PET in men who had undergone a radical prostatectomy but had experienced a recurrence of their cancer. Their findings indicate that PSMA PET should be strongly considered both before initial treatment in men with high-risk cancers and in cases of cancer recurrence after surgery or radiation to provide more precise care. The PSMA tracer also can be used in conjunction with CT or MRI scans.
Watch: What is PSMA-PET Scan Radioactive Imaging?
UCSF and UCLA are the only two medical centers in the U.S. that can offer PSMA PET to the public through this FDA approval. A limited number of other U.S. medical centers are currently using PSMA as an investigational technique, generally as part of a clinical trial. However, more hospitals will have the opportunity to adopt the technology after applying for expedited FDA approval, which is now possible as a result of the initial FDA approval gained by UCLA and UCSF.
“I believe PSMA PET imaging in men with prostate cancer is a game changer because its use will lead to better, more efficient and precise care,” said Peter Carroll, MD, MPH, a professor at the UCSF Helen Diller Family Comprehensive Cancer Center.
“Prostate cancer is one of the most common cancers in men, with more than 190,000 newly diagnosed cases expected just this year alone,” said Johannes Czernin, MD, chief of the Ahmanson Translational Theranostics Division at UCLA. “That’s why this major effort between the UCLA and UCSF nuclear medicine divisions and our many partners was important and will significantly change for the better how this cancer is detected and treated.”
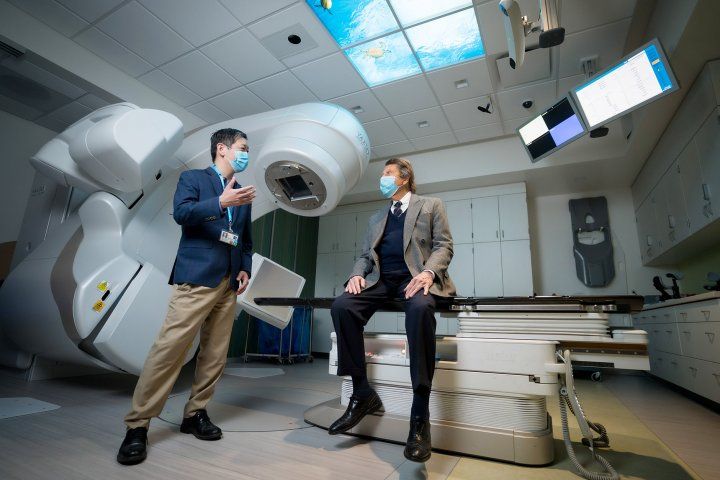
Felix Feng (left), MD, with patient Dennis Brod, in a radiation treatment room at the UCSF Precision Medicine Cancer Building in Mission Bay. Photo by Maurice Ramirez
The UCLA research team was led by the nuclear medicine faculty from the molecular and medical pharmacology department’s Ahmanson Translational Theranostics Division. They worked in collaboration with the departments of urology, radiation oncology and radiology, along with support from the Geffen School of Medicine, the UCLA Jonsson Comprehensive Cancer Center and the Prostate Cancer Foundation.
The UCSF research team was led by faculty from the molecular imaging and therapeutics section of the department of radiology and biomedical imaging, who worked in collaboration with the departments of urology, radiation oncology and medical oncology. Support was provided by the UCSF Helen Diller Family Comprehensive Cancer Center and a philanthropic gift to the UCSF Department of Urology, and by the Prostate Cancer Foundation.
“‘Game changer’ is almost an understatement for how prostate cancer patient care could be improved by this technique,” said Jonathan W. Simons, MD, CEO of the Prostate Cancer Foundation. “After investing more than $26 million in research on PSMA over many years, we are honored to congratulate the research teams at UCSF and UCLA on their milestone achievement.”
For information about PSMA PET patient care, visit UCLA and UCSF websites.
The UCSF Helen Diller Family Comprehensive Cancer Center (HDFCCC) integrates the work of researchers and clinicians who are dedicated to four fundamental pursuits: laboratory research into the causes and events of cancer’s progression; clinical research to translate new knowledge into viable treatments; compassionate, state-of-the-art patient care; and population research that can lead to prevention, early detection, and quality-of-life improvement for those living with cancer. The HDFCCC holds the National Cancer Center’s designation as a comprehensive cancer center. The Center’s 420-plus members and associate members represent dozens of departments and institutes across UCSF, which is the only University of California campus devoted exclusively to the health sciences. Members are faculty investigators in laboratory, clinical, and population-based research who collaborate across the cancer spectrum, from basic biology to risk factors and prevention and control strategies. For more, visit cancer.ucsf.edu.
The UCLA Jonsson Comprehensive Cancer Center is a leader in cancer care, research and education. Our more than 500 physicians and researchers develop new therapies, diagnostics and other technologies, and work to advance our understanding of the disease. We do this while remaining patient-focused and providing the best cancer care possible. As one of only 51 comprehensive cancer centers designated by the National Cancer Institute, we have the resources on our campus, through our community clinics and with our partners, to treat even the toughest cancers and discover new ways to prevent and eliminate this disease. To learn more, visit cancer.ucla.edu.