UCSF Expands Courses on How to Be an Anti-Racist Scientist or Clinician
In most hospitals around the country, an estimation of a patient’s kidney function, known as the eGFR, is adjusted higher if the patient is Black. This “race correction” is built into electronic health records and taught in medical schools, but traces its origins to the racist assumption that Black people have more muscle mass. In practice, this race-based adjustment risks overestimating a Black person’s kidney function and delaying referrals to specialists, treatments and even transplants.
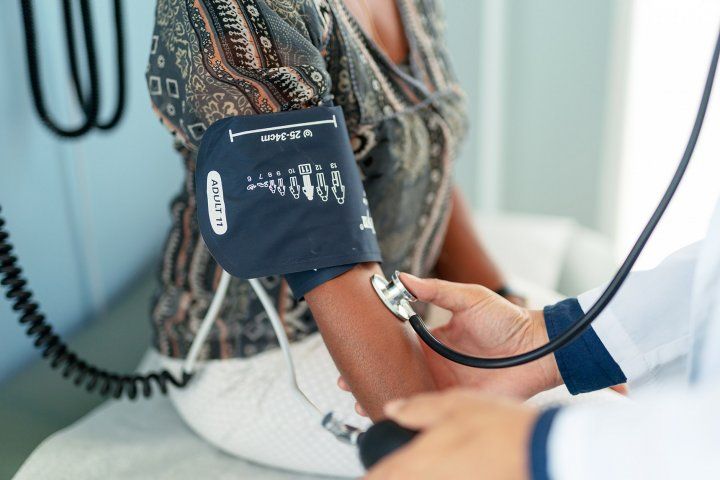
"Race corrections" used in medical algorithms can result in less medical care for minority patients compared to white patients.
This year, UC San Francisco hospitals and Zuckerberg San Francisco General Hospital ended eGFR reporting by race, becoming some of the first hospitals in the country to do so.
The change is part of a growing awareness of racism in medicine and health research, and a movement to train the next generation of clinicians and scientists in ways to counter racism in their professions.
The events of this year – from COVID-19’s disproportionate toll on communities of color to the documented police killings of Black men and women – have accelerated the calls for anti-racism education.
In response, UCSF schools have created new courses and expanded existing curriculum that address issues of structural racism in science and health care. They take an explicitly anti-racist approach, which advocates for interventions against racism instead of merely being not racist.
Myths of Race-Based Medicine
The eGFR is just one example of the prevalence of race-based medicine and the harm it can cause. Other “race corrections” in medical algorithms deem a person identified as Black to have lower risk of heart failure, higher risk of complications from cardiac surgery, higher risk of complications from vaginal birth after a cesarean section, and lower risk of kidney stones.
The rationale for these adjustments are often murky, but they tend to result in less medical care for patients of other races compared to white patients.
Racial bias even extends to medical devices. Spirometers, which measure lung capacity, have buttons that lower the threshold for normal readings for Black and Asian patients, under the assumption that they naturally have less lung capacity than white people. Pulse oximeters have trouble measuring blood oxygenation through darker skin. Even automatic soap dispensers sometimes fail to recognize darker hands.
The persistent myths of race-based medicine can perpetuate health disparities – by undertreating pain in Black patients, for example – but are still taught to new health care professionals.
The Family Nurse Practitioner program in the School of Nursing is in its second year of offering a course on Racism, Health Care and Social Justice, taught by Lisa Mihaly, RN, MS, FNP, and Jayme Mejia, RN, MSN, FNP. In the first lecture, Mihaly shows a slide with myths: that Black and white people need different blood pressure medications, Black people have different pain tolerance than other groups, and renal function varies by race, for example. When she asks how many students have been taught these as fact, an overwhelming majority of students say they have.
When health disparities are reported – the current disparities in COVID-19 infection, for instance – racism is rarely discussed as the root cause, which leaves the impression that there is something inherently wrong with Black and brown bodies – whether biological, genetic, or behavioral - that makes them more vulnerable to disease.
At the heart of these misinterpretations is the enduring myth that race is biological rather than the social and political construct that it is, said Mihaly. Racial categories on the U.S. Census have changed nearly every decade since 1790. Studies have found greater genetic variation within races than between them. Yet in science and medicine, racial categories are still widely used as a shorthand for biological differences. Race as a shorthand for biology is not only inaccurate, it’s dangerous, said Mihaly.
Confronting Racism in Health Care
Racism, Health Care and Social Justice is among the new course offerings that name the role of racism and other forms of oppression in health care. In designing the course, which is a significant revamp of a previous course called Vulnerable Populations, Mejia said, “we decided to be more intentional about naming structural racism and moving away from approaches, common in nursing and medical care, that blamed the individual for their poverty and illnesses.” The lectures and discussions tackle racism, xenophobia, homelessness, environmental justice, reproductive justice, and more.
Mihaly, who was a policy advocate before going to school for nursing, said the class also prepares students with advocacy skills to help make change in their own communities and on state and federal levels.
“As health care providers, there has been a tendency to stand back and say, ‘That’s not ours to fix, we can only deal with what comes into our exam room,’” she said. “I think it’s clear to us that as health care providers, we have to address racism because it affects our patients so profoundly.”
This year, the course will also be open to Pediatric Nurse Practitioners, with the addition of Linda Stephan, RN, MSN, PNP, as an instructor. The midwifery program also has been offering a similar course, Racism and Health Disparity Prevention, since 2014, started by Kim Quang Đâu, RN, MS, CNM, and currently taught by Ifeyinwa Asiodu, RN, PhD. A group of students who took the new course last year are advocating to make it a requirement for all students in School of Nursing.
As health care providers, there has been a tendency to stand back and say, ‘That’s not ours to fix, we can only deal with what comes into our exam room,’” she said. “I think it’s clear to us that as health care providers, we have to address racism because it affects our patients so profoundly.
The School of Medicine plans to weave in more anti-racism and social justice content throughout its curriculum. The BRIDGES curriculum, launched five years ago, introduced anti-racism material in two courses for first-year students, Health and the Individual and Health and Society. The three-week courses focus on social and behavioral sciences, social justice and structural racism, said instructor Megha Garg, MD, MPH.
This year, to make room for more in-depth anti-racism content in these two courses, some introductory lectures on health disparities and racism in medicine will be moved to earlier blocks in the curriculum that focus on basic and clinical sciences. That means making sure all instructors, whether they specialize in cardiology or anatomy, can teach from an anti-racism framework.
“The new paradigm of medical education is to understand that the disparities in outcomes for patients are completely predicated on our racist structures and policies that have existed in this country for centuries,” said Garg. “What we might have previously blamed on non-compliance or completely inaccurately said was a genetic predisposition to certain diseases, we are learning are the result of our structural housing policies, for example, and the biases we’ve had especially toward Black and indigenous people in this country.”
“And it’s not enough to just say that the disparities exist, but we are recognizing that we as a medical profession have to do something about it.”
Lessons from History
In the Graduate Division, in response to specific student demands, all first-year students this fall will have the opportunity to take Racism in Science, taught by Aimee Medeiros, PhD, a historian who studies race and racism in American medicine. The course will cover the history of racism in scientific research, the impact of bias and lack of diversity in science, and what it means to be an anti-racist scientist.
Though the course is not required, demand for the course was high with some 150 students signing up, so many that the course had to be split into two sections.
“Scientific research might seem like it’s a world from anti-racism, but I’m hoping the course will help students see the way in which anti-racism could be possibly applied to one’s professional identity,” said Medeiros.
In the spring, the Graduate Division is also offering three-week mini-courses on Racism in Research, taught by UC President’s Pre-Professoriate Fellows, who are graduate students in the Department of Humanities and Social Sciences. These smaller classes will dive deeper into specific areas – such as the history of epidemics and their impact on marginalized communities or LatinX health issues – that are the focus of the fellows’ research.
Scientific research might seem like it’s a world from anti-racism, but I’m hoping the course will help students see the way in which anti-racism could be possibly applied to one’s professional identity.
Antoine Johnson, one of the fellows, said clear throughlines connect eugenics in the early 20th century with hysterectomies in ICE detention centers today, or the Tuskegee syphilis experiment from 1932 to 1972 with the undertreatment of pain for Black patients today.
“I think there’s this optimistic idea that scientific advancement will self-correct for racial bias because it’s inherently objective, but I think what we’re trying to teach is that these biases persist despite that, even today, sometimes in subtle ways,” said Carlos Martinez, another fellow. “But we need to challenge these racial biases head on and address them.”
Learning about the mistakes and biases of past scientists can help future scientists see their own. “In phrenology, we can look back and see how they were so motivated by their ideas of racism that they led them to certain conclusions – and I’m not so sure that we’re in a place where we’re immune to that,” said Medeiros.
The advent of genomic research has seen a resurgence of race-based medicine, with scientists searching for genetic explanations for poor health in marginalized communities. These inquiries again rely on the faulty concept of biological race while giving short shrift to the social factors that largely account for these disparities.
Anti-Racism in Action
It’s important for basic science graduate students to keep in mind these pitfalls as they go forward in their careers, said Medeiros. In the lab, that could mean understanding that inequities are not natural, or recognizing that races are not biological categories.
In the clinic, too, understanding the long shadow of historical racism in medicine can help UCSF clinicians-in-training be anti-racist in their interactions with patients. Kathy Kemp, a family nurse practitioner student who took Racism, Health Care and Social Justice last year, said that learning about how J. Marion Sims, sometimes known as the father of obstetrics, experimented on enslaved women, practicing on their bodies without anesthesia in order to better treat white women, made her consider her own role as a student-clinician.
“I didn’t want to be someone who was practicing on vulnerable populations so that I could be a good provider,” she said.
Because of what she learned in class, she is more careful about clearly identifying herself as a student-clinician and asking patients whether they prefer seeing a non-student.
Though students arrive at UCSF with varying exposure to and understanding of the problems of racism in science and medicine, it’s undeniable that racism persists in the practice of science and health care, including the way they are taught in many schools.
Nursing textbooks still have pages describing stereotypical behaviors of patients of different ethnicities – under the guise of teaching cultural competency. Even though this is not part of the nursing curriculum at UCSF, nursing students are still tested on these ideas in their licensing exams.
Anti-racism also means starting conversations with peers, colleagues, and those in positions of power.
Anti-racism courses give students a time and place to engage with these difficult, often personal topics, said Medeiros. She acknowledged that some students may feel more burdened by the issues of racism and oppression discussed in class. An added challenge this year, is conducting these discussion-heavy courses remotely over Zoom.
“I think places like UCSF are at the forefront of changing these conversations. I think that this is the wave of the future. This is what the fix is. The future of medicine is anti-racist, whether people like it or not,” said Garg.
“I think we’re ahead of the curve,” said Mejia, “But also it’s long overdue.”