3D Facial Scans Could Speed Diagnoses for Children with Rare Genetic Diseases
Researchers from Alberta, California and Colorado Combine 3D Imaging and Machine Learning to Create Prototype Diagnostic Tool
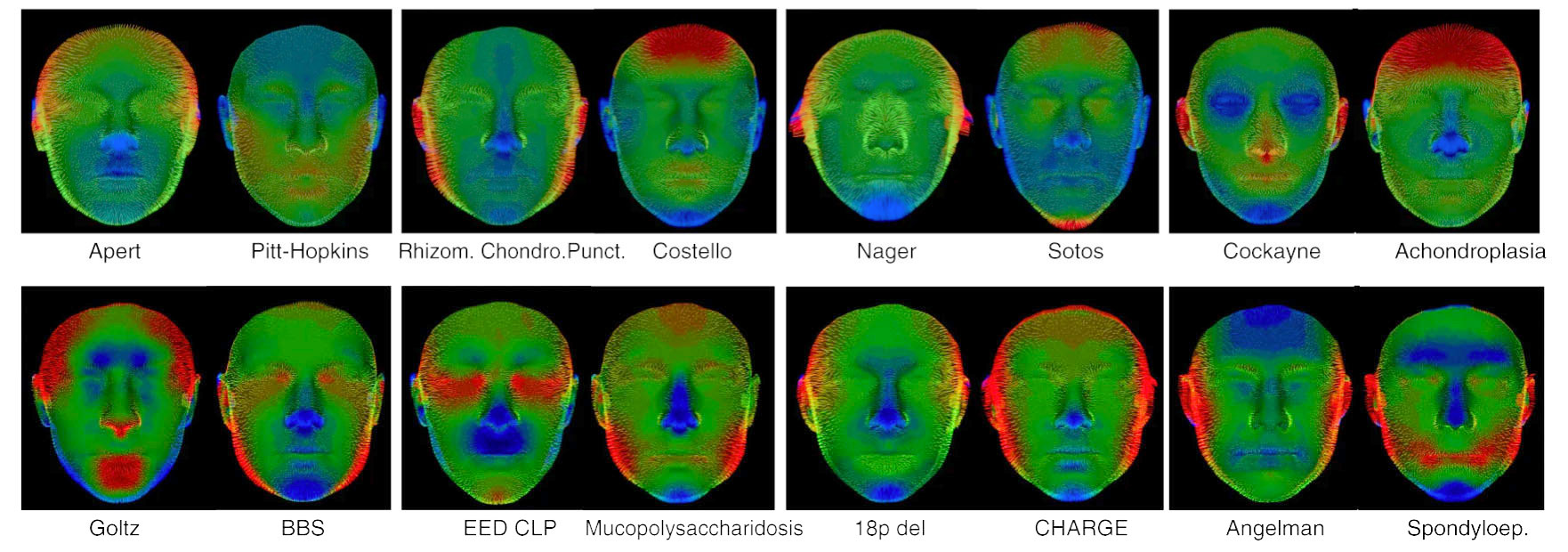
A machine learning algorithm analyzed thousands of 3D facial images in a secure database to ID aspects of facial shape and structure that differentiate hundreds of genetic syndromes. Shown here are computer-generated images illustrating facial features that distinguish different syndromes. Image credit: Genetics in Medicine
Most children with rare genetic diseases spend years undergoing medical tests and waiting for a diagnosis – a long, exhausting process that takes its toll on children and their families. Almost half of these children never get a definitive diagnosis.
Now an international team led by scientists and clinicians from the University of Colorado, University of Calgary, and UC San Francisco has developed a prototype tool based on 3D facial imaging that could shorten that diagnostic odyssey by making it easier for clinicians to diagnose genetic syndromes.
“Families tell us having a diagnosis for their child’s rare disease is life-changing,” said Benedikt Hallgrímsson, PhD, professor and head of the Department of Cell Biology & Anatomy, and scientific director (basic science) at the Alberta Children’s Hospital Research Institute in the Cumming School of Medicine at the University of Calgary. “A diagnosis is essential to children getting the right treatments and connecting with other children and families with the same syndrome.”
Most developmental genetic syndromes affect multiple organ systems, and clinical geneticists have long relied on distinctive facial features as an important guide to diagnosis.
In a new study published online in Genetics in Medicine on June 1, 2020, the research team created a unique library of 3D facial images of participants of diverse ages and ethnicities, including 3327 children and adults with 396 different genetic syndromes, 727 of their unaffected relatives and 3003 other unaffected individuals from the United States, Canada, and the United Kingdom. The secure database is hosted by FaceBase, an international consortium funded by the National Institute of Dental and Craniofacial Research, part of the U.S. National Institutes of Health (NIH).
The researchers then used this secure database to train a machine learning algorithm to identify most of the genetic syndromes included in the dataset with moderate-to-high accuracy. Based on facial shape, 96 percent of study subjects could be correctly classified as either unaffected or having a syndrome, and for most, the algorithm was able to provide a prioritized list of likely diagnoses with high accuracy.
The COVID-19 pandemic has accelerated a rapid shift to telemedicine by genetics clinics, including those at UCSF, University of Colorado, and University of Calgary, but the study team says the field still lacks tools to replace many aspects of the in-person physical exam. The automated diagnostic approach developed in this study could extend the ability of clinical geneticists to diagnose patients without requiring travel to a specialized clinic. It could also help general practitioners without genetic training to home in on potential diagnoses, enabling them to connect patients with appropriate specialty care and community support.
“Clinical genetics is labor-intensive,” said Ophir Klein, MD, PhD, the Larry L. Hillblom Distinguished Professor in Craniofacial Anomalies and the Charles J. Epstein Professor of Human Genetics at UCSF, where he is chief of the Division of Medical Genetics. “Some clinics have a two-year waiting list to get in. Using 3D imaging could dramatically enhance clinicians’ ability to diagnose children more quickly and inexpensively.”
The researchers emphasize that the current study represents an important proof-of-concept for facilitating genetic diagnoses, but further work is required to deploy a clinically available, privacy-protected tool. Currently, the approach relies on expensive 3D cameras, but this is expected to change with advances in smart-phone camera technology.
“We have designed a prototype with significant potential to become a clinical tool around the world,” said Richard Spritz, MD, professor of Pediatrics and director of the Human Medical Genetics and Genomics Program at the University of Colorado School of Medicine. “Our hope is that one day soon, our patients can securely take a photo of their face with a smart phone and send it to their doctor for analysis in a confidential database.”
Added Hallgrímsson, “In low-income countries where genetic testing and medical geneticists aren’t available, this could become a transformational new tool.”
Corresponding Authors: Benedikt Hallgrímsson is professor and head of the Department of Cell Biology & Anatomy, a professor in the Department of Radiology, scientific director (basic science) at the Alberta Children’s Hospital Research Institute and a member of the McCaig Institute for Bone and Joint Health.
Ophir Klein is professor in the departments of Orofacial Sciences and of Pediatrics, the Larry L. Hillblom Distinguished Professor in Craniofacial Anomalies, and the Charles J. Epstein Professor of Human Genetics at UCSF. He serves as Chief of the Division of Medical Genetics, Chair of the Division of Craniofacial Anomalies, Medical Director of the Craniofacial Center, and Director of the Program in Craniofacial Biology.
Richard Spritz is professor of pediatrics and director of the University of Colorado School of Medicine Human Medical Genetics & Genomics Program.
Funding: The research was supported by the U.S. National Institutes of Health (NIH), the Alberta Children's Hospital Foundation through the Alberta Children’s Hospital Research Institute, and The Larry L. Hillblom Foundation.
Disclosures: The authors declare no competing financial interests.
About UCSF: The University of California, San Francisco (UCSF) is exclusively focused on the health sciences and is dedicated to promoting health worldwide through advanced biomedical research, graduate-level education in the life sciences and health professions, and excellence in patient care. UCSF Health, which serves as UCSF's primary academic medical center, includes top-ranked specialty hospitals and other clinical programs, and has affiliations throughout the Bay Area. Learn more at ucsf.edu, or see our Fact Sheet.
About the University of Calgary: The University of Calgary is a global intellectual hub located in Canada’s most enterprising city. In our spirited, high-quality learning environment, students thrive in programs made rich by research, hands-on experiences and entrepreneurial thinking. Our strategy drives us to be recognized as one of Canada’s top five research universities, engaging the communities we both serve and lead. This strategy is called Eyes High, inspired by the university's Gaelic motto, which translates as 'I will lift up my eyes.' For more information, visit ucalgary.ca/eyeshigh.
About the University of Colorado School of Medicine: The University of Colorado Anschutz Medical Campus is the largest academic health center in the Rocky Mountain region, and a world-class medical destination at the forefront of transformative education, science, medicine, and healthcare. The campus includes the University of Colorado health professional schools, multiple centers and institutes and two nationally ranked hospitals, UCHealth University of Colorado Hospital and Children’s Hospital Colorado, which treat nearly 2 million patients each year. All interconnected, these organizations collaboratively improve the quality of patient care they deliver, research they conduct, and health professionals they train.