This article is archived and only made available for historical reference. If you’d like to discover UCSF’s most recent advances in research, education and patient care, please visit the UCSF News Center.
Archive: New Standards to Improve Diagnosis of Sjogren's Syndrome
UCSF-Led Team of International Researchers Develop Criteria to Identify Autoimmune Disease
Sjögren's syndrome largely was unknown to the American public until tennis star Venus Williams withdrew from the U.S. Open last year and announced she had the autoimmune disease, in which a person’s white blood cells attack glands that produce tears and saliva.
Now, new guidelines have been developed by an international consortium of researchers, led by those from UCSF, to better support diagnosis and genetics research of Sjögren’s syndrome. It’s the first time the American College of Rheumatology (ACR) has approved classification criteria for the disease.
The criteria are outlined in the article, “American College of Rheumatology Classification Criteria for Sjögren’s Syndrome: A Data-Driven, Expert Consensus Approach in the Sjögren’s International Collaborative Clinical Alliance Cohort,” published in the journal Arthritis Care & Research.
As many as 4 million Americans are living with this disease, according to the Sjögren’s Syndrome Foundation. It’s the second-most common autoimmune rheumatic disease in the United States, with women representing 90 percent of those affected.
The effects from the dryness they experience can be quite significant.
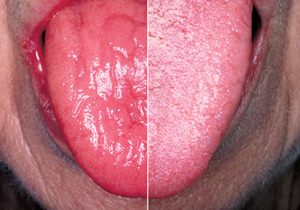
A duplex image of a patient's tongue with Sjögren's syndrome, before treatment on the left and after treatment on the right.
“Tooth decay may be one of the signs which actually makes a dentist suspect that a patient has Sjögren's syndrome,” said co-lead author of the study Caroline Shiboski, DDS, PhD, professor of oral medicine at UCSF School of Dentistry. “Such dramatic tooth destruction can be prevented with early diagnosis of salivary hypofunction and prescription of topical fluoride.”
Diagnosis and management of Sjögren’s syndrome requires three areas of specialty practice: rheumatology, ophthalmology and oral medicine/pathology.
Until now, doctors diagnosing the disease relied on a combination of objective tests and subjective features such as patient reports of signs and symptoms.
“Some of the subjective manifestations of Sjögren's syndrome — dry eyes and dry mouth — are so non-specific,” said Lindsey Criswell, MD, MPH, chief of the UCSF Division of Rheumatology. “In previous years, when those common and non-specific symptoms were part of the classification criteria, some of those patients indeed had Sjögren's syndrome, but others who met those criteria probably had something else.”
The Sjögren’s International Collaborative Clinical Alliance (SICCA) was created to develop a simpler and more objective criteria set, establishing a universal standard for Sjögren's syndrome.
"This new criteria set provides more clarity and specificity, which is particularly important for clinical trial enrollment," said co-lead author Steve Shiboski, PhD, professor at the UCSF Division of Biostatistics. "Correct classification of individuals without the disease helps avoid unnecessarily exposing them to potentially toxic side effects of some experimental treatments."
A Universal Standard
The definition of Sjögren's syndrome has evolved as researchers’ understanding of the disease improved.
“This isn’t a disease localized to the eye or localized to the mouth and teeth; it’s a systemic disease,” Criswell said. “With that recognition, different specialty groups have been coming together to try to develop criteria that encompass all of those manifestations.”
As described in the published article, the SICCA project — comprised of experts from ophthalmology, rheumatology and oral medicine – agreed on a methodology to define the target population and identify and select the criteria. This was followed by a series of validation exercises from a data-based approach.
“In past research studies using earlier criteria, which allowed various symptoms and tests for disease classification, results could be variable, leading to inconsistent results,” said Troy Daniels, DDS, MS, professor of oral medicine and pathology at the UCSF Schools of Dentistry and Medicine and a founder of the UCSF Sjögren’s Syndrome clinic in 1972. “I think that a great deal of past research has been well conceived but the specimens coming into the studies were from inadequately classified sources.”
The Criteria
Tests for the new classification criteria include:
- Anti-SS-A/B serology, which measures the level of specific Sjögren’s syndrome antibodies in blood.
- Labial salivary gland biopsy — the removal of minor salivary glands from the lips — which demonstrates a specific pattern of inflammation associated with Sjögren’s syndrome.
- Staining the eye’s surface with a specialized dye to test keratoconjunctivitis sicca, an eye disease caused by eye dryness. A score of three or more is considered to be positive.
Two of the three tests must be positive for a person to be diagnosed with Sjögren’s syndrome.
The next step will be to collaborate with representatives of the European League Against Rheumatism (EULAR), the European equivalent of ACR, to perform additional validation involving a European cohort with the goal of achieving a single international standard.
Ultimately, researchers hope a universal standard could lead to faster and more accurate diagnosis of Sjögren's syndrome.
“The prevention of complications is a very important reason why Sjögren's syndrome should be better understood by clinicians and the general public,” Caroline Shiboski said.
Funding support was provided by the National Institutes of Health (NIH) specifically the National Institute for Dental and Craniofacial Research, National Eye Institute and Office of Research on Women’s Health.