International Surgeons Learn Life-Changing Procedures from UCSF/SFGH Surgeons
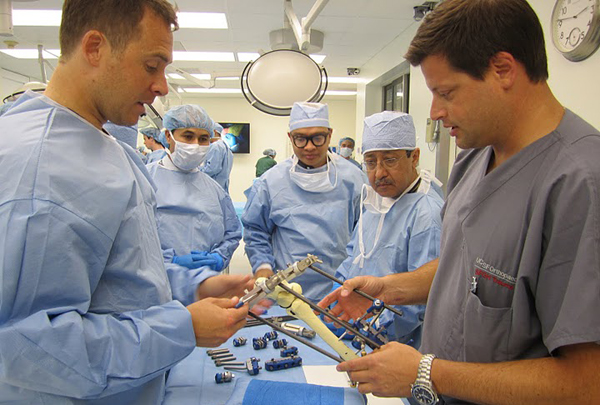
Surgeons from 17 different countries, including Jair Kimri Jingco, center, an orthopaedic surgeon from the Philippines, participated recently in hands-on training offered by the Institute for Global Orthopaedic & Traumatology. Scott Hansen, MD, right, assistant professor of plastic, reconstructive and orthopaedic surgery, is among the instructors.
Jair Kimri Jingco, MD, peers attentively through his black-rimmed glasses, his eyes transfixed on a surgical procedure being demonstrated in front of him.
He is one of a dozen surgeons huddled around an operating table at a cadaver lab in the Institute for Global Orthopaedics & Traumatology (IGOT) located at San Francisco General Hospital (SFGH) and Trauma Center. IGOT was started by faculty and residents in the UCSF Department of Orthopaedic Surgery to provide training to surgeons to ease the burden of musculoskeletal injuries, especially for underserved populations in developing countries.
Jingco, a 35-year-old orthopaedic surgeon from Bacolod City, Philippines, observed a hands-on lesson in how to treat bone fractures and open injuries taught during IGOT’s second annual orthopaedic flap course held Sept. 11 through 13.
A flap – a piece of tissue partly detached from its place of origin to cover exposed bones or tendons – is used by surgeons in severe trauma cases, to try to save the limb. UCSF surgeons at SFGH are only a handful in the country who teach flap techniques to surgeons from around the world.
For training purposes, UCSF surgeons have developed a comprehensive course on a variety of flap techniques for upper and lower extremities, which include didactics and cadaver tissue dissections. The dissection instruction includes the use of cadaver tissues injected with dyes to demonstrate the location of the blood supply to the visiting surgeons.
Jingco traveled almost 7,000 miles to arrive in San Francisco. But his long trek could lead to a major shift in how bone fractures and soft tissue injuries are treated in his homeland. Jingco is only one of seven orthopaedic surgeons in the Visayas region, which has a population of almost 300,000.

Richard Coughlin, MD
Treating soft-tissue defects by using flap work is a relatively novel concept in the Philippines. Adequate training for these types of procedures is not available in many developing countries. The first procedure was performed there just a year ago, and the success rate so far has been low: around 25 percent.
“If you do it and mess up, you may not have another chance for surgery,” Jingco said. “The patient might give up and go home.”
Toll of Traumatic Injury in Developing Countries
About 5 million people die from trauma each year globally, and up to 45 million are permanently disabled by trauma. Ninety percent of all injuries occur in developing countries, according to the World Health Organization.
“When you think of a poor farmer or a laborer who experiences a traumatic injury, their family is devastated,” said Richard Coughlin, MD, IGOT’s director who led efforts to bring this symposium to San Francisco. “They’re trying to feed him every day and he’s in a hospital for three months. That screams inequity.”
That’s a scenario all too familiar for Raphael Kumah, MD, an orthopaedic surgery chief at Komfo Anokye Teaching Hospital in Kumasi, Ghana. He has seen patients whose injured limbs had to be amputated because hospitals in rural areas were not equipped to handle complex orthopaedic cases.
“It’s a significant impact economically, socially, physically because you will be physically challenged,” he said. “In a society where most people survive on physical labor, if they lose a limb, that’s a major problem.”
By holding international symposiums like the one held last week, IGOT hopes to improve trauma care and to reduce the number of amputations performed in developing countries, according to Theodore Miclau, MD, chief of orthopaedic surgery at SFGH, vice chair and director of orthopaedic trauma of the UCSF Department of Orthopaedic Surgery, which is internationally recognized for its work in patient care, education and research.

Theodore Miclau, MD
“It’s not just a matter of us sending a surgeon there to operate on a group of patients and then leave,” Miclau said. “It’s really to develop programs where the surgeons who are there and the health care providers who are there can be educated and build their own capacity.”
“It’s a labor of love; it’s a labor of commitment. This is who we are as professionals,” added Coughlin. “Our greatest hope is that our efforts are actually met with improved outcomes.”
Making a Difference Through Training
IGOT’s work is already making a difference.
“Because of my training last year, I was able to email one of the plastic surgeons here and ask for his advice on a complicated case,” Jingco said. “He made recommendations. We followed them and it worked!”
Coughlin hopes this example can be multiplied many times over in Afghanistan, Bangladesh, Cameroon, Ecuador, Ethiopia, Ghana, Haiti, India, Malawi, Myanmar, Nepal, Nigeria, Pakistan, the Philippines, Sierra Leone, Tanzania and Uganda – the 17 nations represented at this year’s IGOT symposium.
“These guys are doing these flaps and they’re also going to teach their residents to do this procedure and change their hospital system to be able to better manage injured patients and raise their standards,” he said.
A new class offered this year was a course on basic clinical research methodology, a resource lacking in many developing countries.
“The idea behind it is in addition to enriching the training of these surgeons from around the world, we wanted to empower them,” said Saam Morshed, MD, MPH, director of clinical research at the Orthopaedic Trauma Institute at UCSF. “We want to help local surgeons develop capacities to develop sustainable programs.”
The research course is a major reason why Jingco returned for a second year. He wanted to learn from this vast network of surgeons and hopefully publish a paper one day with his mentors.
“I tell my residents these are some of the best in the world and they’re willing to collaborate with us,” Jingco said. “If we show diligence, if we show enthusiasm, and if we can show them that we can actually pull it off, they’d work with us and new doors could open.”
Improving Health Care Worldwide
As Kumah travels 7,561 miles back to Ghana, he carries home new knowledge and a sense of renewed optimism.
“My hope is that in the next four to five years, we train enough doctors to be able to have this expertise and spread the knowledge of orthopaedic trauma care,” he said. “It’s a great joy. It is a noble calling to save limbs.”
For Coughlin, his long-term vision of helping the world also benefits the San Francisco Bay Area community.
“It’s here in this city. It’s in this neighborhood,” he said. “It’s in Northern California where we get referred in patients who basically are here because other places don’t want to deal with them.”
Coughlin hopes the momentum generated with this symposium will snowball. “This isn’t just idealism; this is real. We are dramatically improving health care worldwide.”