University of California San Francisco
Give to UCSFBrain Tumor Surgery that Pushes Boundaries Boosts Patients Survival
Survival may more than double for adults with glioblastoma, if neurosurgeons remove the surrounding tissue as aggressively as they remove the cancerous core of the tumor.
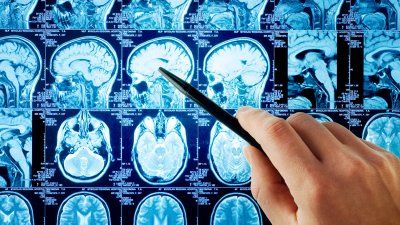
As Mysterious Coronavirus Spreads, An Infectious Disease Expert Explains What You Should Know
Just weeks since the viral illness was first reported in Wuhan, China, health experts globally are working on containing and treating it.To put the latest news in context, we asked UCSF infectious disease expert Charles Chiu, MD, PhD, about the origins of the Wuhan virus and public health risks going forward.
The Infectious Diseases on the Rise – and on the Way Out
Infections that plagued the world for centuries (malaria, HIV/AIDS) are on the verge of eradication. Others threaten to disrupt human lives and economies more than ever before.

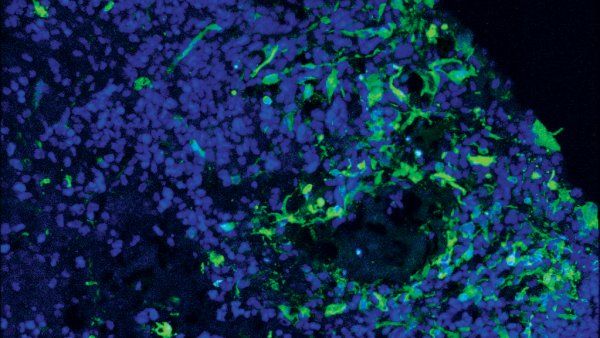
Brain Organoids Reveal Glioblastoma Origins
UCSF postdoctoral researcher for the first time succeeded in keeping a diverse array of glioblastomas alive in the lab using brain organoids
How Scientists Might Tame Cancer
Basic scientist Zena Werb, who has studied cancer cells in UCSF labs for more than four decades, shares her take on the future of cancer medicine.

Who Will Benefit From Precision Medicine?
A future in which precision medicine benefits everyone is not guaranteed. For that to happen, UCSF experts argue, the health care industry must first tackle today’s health disparities, including differences in disease outcomes and access to care based on race, gender, and socioeconomic status.

What Will Health Look Like in 2050?
No one can see the future, but that won’t stop us from trying. We asked UCSF faculty and alumni to score these predictions for likelihood and impact.

Health Care is Going Green
The health care sector accounts for as much as 10% of the U.S. carbon footprint and 5% globally, according to recent studies. This sobering statistic has an upside: It means that changes in the industry can play a major role in addressing the climate crisis.

Climate Change is a Health Crisis
Hurricane. Fires. Disease and allergen outbreaks. Heat waves. These climate-fueled events kill, they pack ERs, and they leave lingering legacies of toxic pollution, pulmonary complications, and post-traumatic stress – but they are just a glimpse of what’s to come unless the world makes an extraordinary course correction.

UCSF’s 11 Most Popular Health and Science Stories of 2019
Browse the stories that most engaged our readers in 2019.
In Childhood Cancer, Private Insurance Means Better Survival
Children and young adults with pediatric cancer are less likely to be alive five and 10 years following diagnosis if their health insurance is public, compared to those with private insurance.
