Research Breathes Life into New Asthma Clinic at UCSF
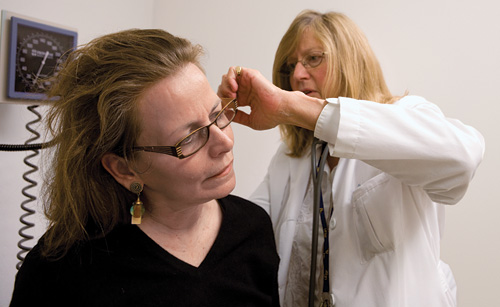
Clinician-researcher Susan Janson sees a patient at the asthma clinic at UCSF Medical Center.
By Andrew Schwartz
More than 20 million Americans suffer from asthma, but hundreds of them now breathe more easily, thanks to a Monday morning asthma clinic that opened its doors in the UCSF Ambulatory Care Center in June 2008.
Combining expert consultation and self-management education services, the clinic emerged in large part from three evidence-based research studies led by clinician-researcher Susan Janson, RN, ANP, DNSc, FAAN.
Janson’s studies are rooted in other established research that found patients better manage their chronic diseases when there is a strong patient-clinician relationship. With that understanding, Janson, professor and Harms/Alumnae Chair of the UCSF School of Nursing’s Department of Community Health Systems, set out in 1993 to discover the most effective way for clinicians in such relationships to deliver the appropriate knowledge and skills about asthma within the constraints of today’s health care delivery system.
Her first study – an open trial funded by the National Institute of Nursing Research – found that during a 30-minute clinic appointment, it was feasible for a nurse to perform an educational intervention that decreased symptoms and reduced biological markers of airway inflammation. The published trial not only encouraged Janson to push ahead, but also had important implications for reimbursement.
“Getting the teaching done in the context of a medical appointment makes it billable because the visit can be coded at the next-higher CPT code if you include teaching as part of total visit time,” says Janson, who stresses that it can sometimes be a challenge to make patient education economically viable.
Her second study – funded by the National Heart, Lung and Blood Institute (NHLBI) – refined the standardized intervention and then tested it in a randomized clinical trial, which also was published. “We tracked study participants for adherence with their use of inhaled steroids, which they weren’t using effectively before,” says Janson.
For those educated in self-management, Janson’s team documented improvement in adherence to inhaled corticosteroid medication and perceived control of asthma, as well as reduced biological markers of airway inflammation. The self-management group also had no emergency department visits for asthma. This is important not just for asthma patients, but also for the medical system as a whole, since every year, asthma cases account for about a quarter of all visits to the emergency room, one of the most expensive areas for delivering medical care.
The third study – also funded by the NHLBI and currently in press – was another randomized clinical trial, this time with a tailored version of the intervention that the team based on the patients’ lung function, category of severity, allergen skin testing responses and specific inhaler technique.
“With personalization, the changes made were significantly greater for all the metrics, including maintenance of medication adherence over time and improvement in the markers of asthma control,” says Janson, who served on the expert panel for the latest NHLBI Asthma Guidelines published in December 2007.
The new guidelines’ focus on controlling asthma includes the use of asthma self -management education by certified asthma educators.
Applying Research
Janson used her study results as the blueprint for the self-management education services provided at the Monday morning asthma clinic at theAmbulatory Care Center. The services have five key components: education about the disease itself; education about how the medicines work; training in how to use the prescribed inhalers correctly; education about how to control aggravating environmental factors; and a personalized, written action plan.

Susan Janson, a professor in the UCSF School of Nursing, is applying her research to benefit patients at a Monday morning asthma clinic.
To target patients who may need these services, Janson collected data on the number of emergency department visits for asthma at UCSF Medical Center because she believes those visits can be substantially reduced if patients are trained in asthma self-management skills. In fact, a key goal in the asthma clinic’s business plan is to help decompress UCSF Medical Center’s emergency department and urgent care clinic.
Janson also expects that educated patients will bring their asthma under control, and that all of the clinic’s patients will be able to demonstrate that they know how to use an inhaler correctly.
To achieve these goals, Janson and respiratory therapist Jack Covington work as a team in a process that is the by-product of 12 years of working together, both clinically and on research projects. In the course of a 30-minute appointment, Janson typically lays the foundation for asthma self-management, after which Covington teaches the inhaler skills and how to follow the action plan.
This can be more difficult than it sounds. There are many different inhalers, each of which requires different skills. And every time there’s a new medication, there’s a new inhaler device, with both needing to pass US Food and Drug Administration requirements. Consequently, says Janson, “Many patients make fundamental errors with their inhalers that prevent deposition of the drug in the airway, largely because they haven’t been taught properly.”
In addition, the education must help patients understand the often complex mix of environmental factors that exacerbate their asthma. Allergens, irritants like tobacco smoke or household products, and co-morbid conditions like sinusitis and allergic rhinitis all can play a role. The strategy for managing exposure to these irritants is unique to each patient, making tailored education all the more critical.
Finally, clinical consultations complement the self-management education of the Monday morning clinic. Janson and the asthma clinic’s physician, Homer Boushey, MD, chief of Asthma Clinical Research Center, who is also Janson’s longtime research collaborator, provide these consultations in response to requests from clinicians within UCSF and from community physicians ranging from the San Francisco Bay Area to California’s Central Valley. Usually the consults involve making treatment recommendations, but they can also include making a definitive asthma diagnosis for those who are less familiar with the appropriate tests, such as spirometry.
“Sometimes we find it’s not really asthma, but severe sinusitis, and we’ll do the necessary tests here to determine that,” says Janson.
Having established a clear pattern of rapidly moving research findings into clinical settings where they can help patients, Janson’s research program continues. A fourth randomized clinical trial – funded by the NHLBI – is in progress, which tests the asthma control effect of cueing patients’ and clinicians’ collaboration by use of an Internet-based feedback tool showing patterns of lung function. Janson is also writing a new proposal to test technology-enhanced asthma self-management to improve asthma control over the long term.
“Patients with chronic diseases like asthma require support for long-term self-management to prevent the behaviors from waning over time,” she says.
Photos by Elisabeth Fall
Source: Science of Caring, Spring 2009
Related Links: