UCSF team advances probe of neural stem cell-brain tumor link
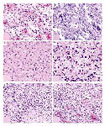
Grades I to IV Astrocytic Tumors -----
The public’s enthusiasm for stem cell research has focused on the potential of the cells to treat disease and traumatic injury. Theoretically, if scientists could deduce how to prompt embryonic or adult stem cells to evolve into the various specialized cells of the body, the cells could be transplanted into patients, replacing, for example, the key brain cells destroyed in Parkinson’s disease.
But below the public radar screen is another element of stem cell research - one focused on illuminating disease. Scientists are studying the earliest stages of embryonic and adult stem cell growth in the culture dish and in animal models with the ultimate goal of identifying the genetic missteps that cause such diseases as amyotrophic lateral sclerosis (ALS), and that account for some cases of birth defects and infertility. Scientists also are conducting studies on adult stem cells to determine whether disregulated stem cells cause some cancers.
In the current issue of New England Journal of Medicine (Aug. 25, 2005), a team of UCSF stem cell scientists and neurosurgeons reports on the increasing evidence from labs around the world that stem cells found in the brain - known as neural stem cells - may be the cause of the most common form of primary brain tumor. These tumors are called malignant gliomas.
Last year, the same team reported the discovery of a ribbon of neural stem cells in the human brain (Nature, Feb. 19, 2004), offering hope that the cells could someday be used to develop strategies for regenerating damaged brain tissue. But at the time, the team, including co-author Mitchel Berger, MD, professor and chairman of the UCSF Department of Neurological Surgery and director of the UCSF Brain Tumor Research Center, also noted that data suggested disregulated forms of these cells could play a role in several disease processes. These include malignant gliomas, the demyelination (or destruction of the protective coating on nerve fibers) associated with multiple sclerosis, and neurodegeneration.
In the current review article, the team examined a body of evidence that they say signals a watershed moment in the convergence of neural stem cell research and brain tumor research.
“At this point, no one can say gliomas arise from neural stem cells. But as we learn more about neural stem cells—where they are located in the brain and how to manipulate them in the experimental setting—we are gaining evidence suggesting a connection between the two,” says lead author Nader Sanai, MD, a resident neurosurgeon at UCSF Medical Center and a neural stem cell researcher in the laboratory of Arturo Alvarez-Buylla, PhD, professor of neurosurgery.
“This paper shows that a significant number of scientists has begun focusing on the possibility. This is why we’re so excited,” he says.
“In the wake of the information explosion that has occurred in the field of neural stem-cell biology,” the team writes in the paper, “a new path is now emerging to link neuro-oncology with developmental neurobiology…Future investigations of human neural stem cells and their potential for malignancy will be indispensable to our continued struggle with brain cancer, since identifying the true source of human gliomas may lead to better therapeutic targeting, the identification of new markers for the progression of gliomas, earlier cancer detection, and the development of new therapeutic agents.”
Malignant gliomas have a dismal prognosis, in part due to the lack of understanding about the cellular origin of the disease, which has thwarted scientists’ efforts to refine treatments and predict tumor behavior.
Much of the current research effort focuses on identifying where in the brain - and by what type of cell - the tumors emerge. In the 1950s, long before it was proven that stem cells existed in the adult brain, studies in animals suggested that gliomas developed in the lining of the brain’s fluid-filled cavity, known as the subventricular zone (SVZ). Rodents exposed to chemicals known to cause genetic mutations associated with gliomas developed tumors in this region. As the tumors grew, they migrated away from the area, toward the brain’s surface.
By the time gliomas are detected in humans, they generally are found in the white matter and, like those found in the rodent studies, are made up of numerous cell types, including astroyctes, oligodendrocytes and, to a lesser extent, neurons.
In the last decade, the discovery that the brain contains neural stem cells has opened up a new landscape for exploration. In humans, the cells have been found in three regions - the SVZ (the discovery in human tissue was made by the UCSF team, Nature, Feb. 19, 2004), the hippocampus (deep in the back of the brain) and the subcortical white matter - a vast region underlying the cortical surface of the brain.
The cells have caught the attention of cancer researchers in part because neural stem cells and the progenitor glial cells they produce (the foot soldiers on the assembly line that leads to the creation of the brain’s three mature cell types—neurons, astrocytes and oligodendrocytes) have many of the same properties as the cancer cells that make up tumors of the nervous system: They proliferate continuously, produce numerous cell types, and are regulated by some of the same genetic pathways active in many brain tumors. As a result, they are capable of exhibiting many of the characteristics of gliomas, says Sanai.
Recently, scientists have shown that if they create certain glioma-associated genetic mutations in neural stem cells and insert them into mice, the neural stem cells begin to display the signs of glial tumor formation.
The gold standard in advancing the theory, however, says Sanai, would be to demonstrate in the culture dish that human neural stem cells could be sequentially modified to form gliomas.
A key to advancing the research at this point is examining human brain tissue, notes Sanai. The UCSF team’s investigation, he says, is being fueled in part by unusual access to this material, as UCSF Medical Center has one of the highest volumes of brain tumor patients in the world and a similarly large human brain tissue bank.
“We’re excited about the work underway because our brain tumor program, combined with the assets of UCSF’s stem cell research and cancer research programs, is providing us with the elements necessary to carry out this work,” he says.
The evidence in the New England Journal of Medicine review indicates, says Sanai, that the “field is picking up speed.” Right now, he says, “there are a handful of groups seriously focusing on the relationship between stem cells and brain tumors. This is probably changing as we speak.”
Links:
August 25, 2005 NEJM article “Neural Stem Cells and the Origin of Gliomas”