QMRI Sees Cartilage Damage Before It’s Too Late
UCSF-Developed Technology is Now Helping Clinicians Detect Early Signs of Osteoarthritis
One in 20 adults suffers from osteoarthritis, caused by wear and tear of the joints. But early signs of the disease – subtle biochemical changes to the cartilage – are invisible to most current clinical imaging techniques, and patients often remain undiagnosed until the damage is irreparable.
Researchers at UC San Francisco’s Musculoskeletal Quantitative Imaging Research Interest Group (MQIR) are pioneering a new technique, known as quantitative magnetic resonance imaging, or qMRI, that can reveal the earliest signs of cartilage damage.
Sharmila Majumdar, PhD, director of MQIR, has been advancing qMRI techniques for more than a decade and is now working to optimize and translate qMRI for clinical applications.
For the last four years, Majumdar’s group has made the technology available to UCSF clinicians, and UCSF is one of only two medical centers in the world where clinicians are now using qMRI to study and develop preventive therapies for osteoarthritis.
Quantifying Cartilage Composition
On an X-ray, degenerating cartilage can only be inferred by studying the space between bones. Standard MRI provides only the morphology of cartilage, and by the time large lesions are visible, the damage is irreversible. QMRI is the only way to provide a detailed assessment of early cartilage degeneration.
Like standard MRI, qMRI uses magnetic fields and sequences of radiofrequency pulses to measure changes in the hydrogen atoms in our bodies – different tissues produce different signals. But while standard MRI produces essentially qualitative images that then must be interpreted by a radiologist, qMRI uses specialized programming to extract quantifiable values out of the image itself.
QMRI allows you to look at cartilage in a healthy enough stage when you can still reverse the damage. That opens up a whole world of interventions.
Associate Professor of Physical Therapy
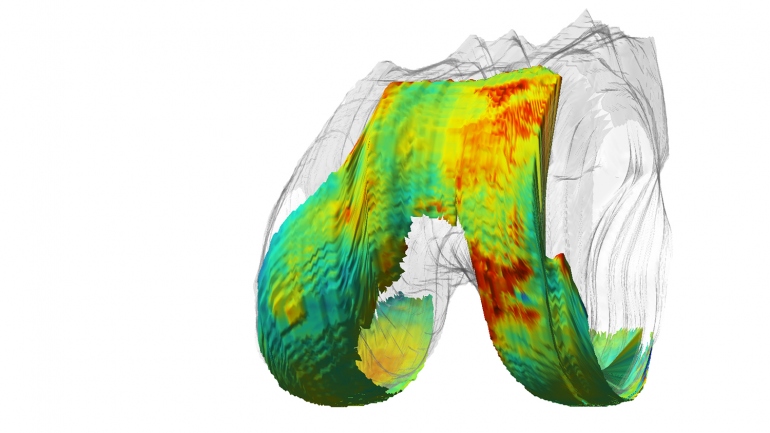
These values are then translated into color scale – producing full color, information-rich images, with red indicating areas of degenerating cartilage.
The technology can detect the early signs of disease in cartilage, including decreased proteoglycan content, increased water content and weakening of the collagen matrix.
“It’s extremely valuable to be able to quantify cartilage composition, because subtle composition changes are reversible,” said Richard Souza, PhD, PT, associate professor of physical therapy. “QMRI allows you to look at cartilage in a healthy enough stage when you can still reverse the damage. That opens up a whole world of interventions.”
Early biochemical changes to cartilage can be healed by reducing stress to the joints through physical therapy or surgery.
As a physical therapist with a background in biomechanics, Souza uses qMRI combined with motion analysis technology to monitor how specific movements, a particular bending of the knee, for example, may exacerbate osteoarthritis. He can help people modify the way they walk and exercise to avoid further damage to the joints.
Early Interventions may Prevent Joint Replacement
Alan Zhang, MD, assistant professor of orthopaedic surgery, sees many young athletes who come in with hip joint pain. He uses qMRI to see if they have early cartilage injury and may recommend surgery to repair tears or remove bone abnormalities to reduce further damage.
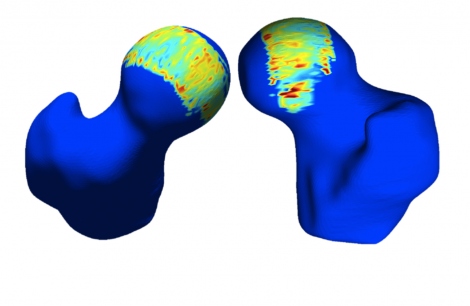
“We’re using qMRI to assess early cartilage injury caused by abnormal boney impingement lesions that may be especially common in the hip,” Zhang said. “Then we may plan surgical interventions to re-contour these lesions or repair certain tears with the goal to prevent the injuries from getting worse.”
Zhang’s clinical research aims to show that these early, minimally invasive interventions can prevent the need for complete joint replacement later on.
QMRI currently is limited to the knee and hip joints, but researchers are working to expand the technique to other joints, such as the ankle and the shoulder, each of which have different surfaces and require different acquisition methods.
Majumdar hopes to speed up data analysis so that images are ready as soon as the patients are out of the scanner. She and Valentina Pedoia, PhD, associate specialist in radiology, are also exploring the possibility of incorporating machine learning methods to allow qMRI to identify patients at risk for joint replacement or those likely to respond to particular interventions.
“In the last 10 years we’ve seen tremendous improvement in imaging equipment and computational resources – but we’re not done,” Majumdar said.